In today’s aging society, many elderly and ailing patients have gradually accepted their long-term care institutions as their second—and sometimes also last—homes, where they pass away. Is it possible for long-term care institutions to execute hospice care? How can long-term care institutions help in the ever-increasing needs of hospice care services? Let’s see what a long-term care institutional expert in Taiwan has to say.
When asked about the beginning of hospice and palliative care, ProfessorChen Hui-zi of Taiwan Long-term Care Professional Association, describes the establishment of St. Christopher's Hospice in the United Kingdom in 1967 by Cicely Saunders, saying, “Hospice and palliative care was indeed started in communities.” The purpose of the institution was very clear from its naming it a hospice instead of a hospital. This building looked simple yet comfortable, and was located in the community. “Its prototype looked very much like the nursing facility in Taiwan today, and similarly, patients can receive hospice and palliative care right in the neighborhood."
Today, most hospice and palliative institutions in the UK are still disbursed throughout the communities, and a large number of private volunteers are called upon to facilitate hospice care at home. Prof. Chen Hui-zi believes that this arrangement is appropriate for the kind of care needed at the end of life “because death is not a medical problem, but a life event. People would still want to live a normal life before leaving the world, even if it's just taking a walk or sipping a coffee."
Hospice Care at Home
Extended from Home Hospice Care
Taiwan’s hospice systems are diverse, and the most utilized form is the hospital hospice care in a hospital’s hospice ward. Another hospice practice also conducted in a hospital is called hospice shared care, in which the hospice team and the original medical treatment team work together to take care of end-stage patients so that patients in regular surgical or medical wards can receive continuous hospice palliative care at the same time.
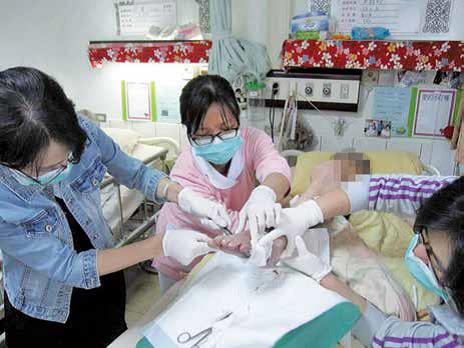 Although hospital hospice care and hospice shared care are more popular in Taiwan, in fact, Taiwan’s hospice began with hospice care at home, just like in the United Kingdom. According to Prof. Chen Hui-zi, "In 1990, Mackay Hospital established the first Taiwan hospice ward of 18 beds, but before that, hospice care at home had already been taking place in Taiwan."
Although hospital hospice care and hospice shared care are more popular in Taiwan, in fact, Taiwan’s hospice began with hospice care at home, just like in the United Kingdom. According to Prof. Chen Hui-zi, "In 1990, Mackay Hospital established the first Taiwan hospice ward of 18 beds, but before that, hospice care at home had already been taking place in Taiwan."
She continues, "In the 1980s, home hospice care had opened for business; at the same time, cancer and serious illness related home hospice care also started developing." Prof. Chen Hui-zi further explained that home hospice care in Taiwan started in church hospitals. For example, Taipei Mackay Memorial Hospital began home hospice care in the 1960s, and Changhua Christian Hospital also made a favorable reputation in the home hospice care in the 1970s. However, the target of the service then was not limited to terminal patients. "The church hospitals at that time didn’t want patients to return home before full recovery; therefore, caregivers were sent to their homes." Prof. Chen Hui-zi, who was one of the visiting nurses in the 1970s, often went to the critically ill patients’ homes to help them return to their normal way of living with dignity.
"Rather than lying in the hospital taking morphine, isn't it better for the patient to stay home?" Back then, Prof. Chen Hui-zi often hopped on the bike and pedaled hard toward a patient’s home. More often than not, before arriving, she could see in the distance the family members waiting anxiously at the door "because only after the morphine injection could the patient have a little strength to eat congee and something else. The injection we delivered could relieve pain so that the patient could gain some energy for life. Although what we started doing in the 1960s and 1970s may not seem like much, it has the same starting point as the current home hospice care.”
In 1997, home hospice care was officially covered by the health insurance program. According to the regulations, after the doctors’ assessment, terminal patients who do not respond well to a variety of therapeutic treatments can apply for home hospice care under certain conditions: that their illness does not require hospitalized treatment, their self-care ability is limited, their time to stay awake exceeds 50%, and their family members have the willingness and ability to care for them and can cooperate with the guidance and implementation related to hospice care. The regulations of the Health Insurance Bureau also state the hospice team professionals will provide home visits in line with the needs of patients. To assist patients alleviate various discomforts and to give family members instructions for relevant care skills, hospice physicians and social workers visit once a week while hospice nurses visit twice a week to ensure that patients enjoy high-quality medical care in their homes.
Missing Part to Complete the Long-term Hospice Care
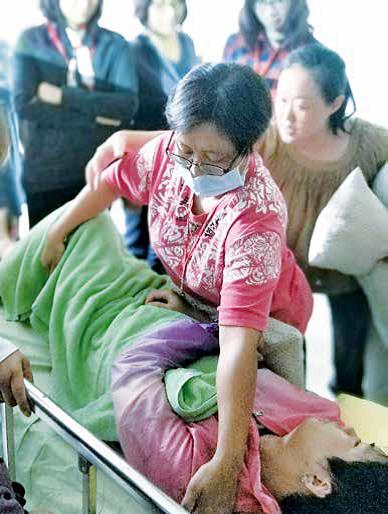 Prof. Chen Hui-zi, who has long been involved in long-term care, believes that with the advent of an aging society, today’s homes are no longer defined in the traditional way. Statistically, there are about 40,000 people currently living in health care institutions and medical care homes in Taiwan. Including those in nursing homes, the total number of people in long-term care institutions is up to nearly 100,000. For these residents, longterm care institutions are their second home, and sometimes their last home. “Some stay there for ten to twenty years so it’s not an exaggeration to call it home."
Prof. Chen Hui-zi, who has long been involved in long-term care, believes that with the advent of an aging society, today’s homes are no longer defined in the traditional way. Statistically, there are about 40,000 people currently living in health care institutions and medical care homes in Taiwan. Including those in nursing homes, the total number of people in long-term care institutions is up to nearly 100,000. For these residents, longterm care institutions are their second home, and sometimes their last home. “Some stay there for ten to twenty years so it’s not an exaggeration to call it home."
Unfortunately, hospice care in long-term care institutions is not supported by health insurance, which deprives the residents of an important way to die well. Prof. Chen Hui-zi sighs, "They often suffer from more than one disease, and the suffering is far beyond imagination. Do these people need hospice care? Absolutely!"
If hospice and palliative care cannot be provided in long-term care institutions, it will become a major gap in hospice and palliative care. For this reason, a few large long-term care institutions in Taiwan have set up hospice beds themselves through fund raising, and, at their own expense, have sent their staff to receive hospice and palliative care training. For example, with 50-60 deaths a year, Zhishan Elderly Care Center has an average of one death almost every week. "Therefore, the hospice beds in Zhishan Center can be said to have a very good utilization rate. However, except for giving hospice care to the elderly three or four days before the end of their lives, what does Zhishan benefit from setting up these hospice beds?” Prof. Chen Hui-zi shakes her head and says, "Nothing."
She further explains that Zhishan Center not only sends its staff to training, but takes care of the hospice patients at its own expense. Although the assigned supporting hospital provides medication, as a long-term care institution, according to the current regulations, it cannot apply for health insurance payments for either the hospice staff or medicine. "This is the most difficult part of promoting longterm hospice in Taiwan today. The organization sees the need of hospice andpalliative care for patients facing end of life. However, some symptom-relieving equipment or medication are unavailable and even if made available by the hospital, will be unaffordable by the organization.
Prof. Chen Hui-zi highlights that at present, there are very few institutions like Zhishan Center, which can set up hospice beds. While large institutions can rely on the strong fundraising power of foundations, there is no solution for small and medium-sized institutions. “They at best move a dying patient to the bed closest to the nurse station. It’s simply impossible to set up a single ward equipped with professional medical equipment."
Turning on the computer, Prof. Chen Hui-zi logs onto the website of St.Christopher’s Hospice. Before the homepage fully loads, a fundraising message has already occupied two-thirds of the screen. Prof. Chen Hui-zi points out, "Even the prestigious St. Christopher’s Hospice has to rely on fundraising to continue with its operations."
However, according to the report of St. Christopher’s Hospice, the annual balance of fundraising and expenditure is always positive. Prof. Chen Hui-zi further analyzes that this is because the British people's general understanding of and support for hospice care have contributed to the prevalence of relevant donations, which, in turn, has led to the widespread hospice care all over the United Kingdom. In contrast, Taiwan’s donations in this regard are not abundant.
Even so, Prof. Chen Hui-zi still holds on to hope, saying, “Today, many in Taiwan who are about to retire will have a high knowledge background. If, like the United Kingdom, they can be guided to participate in hospice education training and volunteer as caregivers in communities, at least there will not be any shortage of manpower in the future.”
Prof. Chen Hui-zi believes that the purpose of understanding and learning of hospice care is not limited to serving others. After all, everyone will face this final stage. The self-awareness and learning they do now will eventually benefit themselves. She concludes, "Taiwan's long-term hospice still has a long way to go, and there are many difficulties to overcome; but perhaps promoting and educating hospice to the people of Taiwan in this day and age will be most beneficial to Taiwan's long term and hospice care.”

