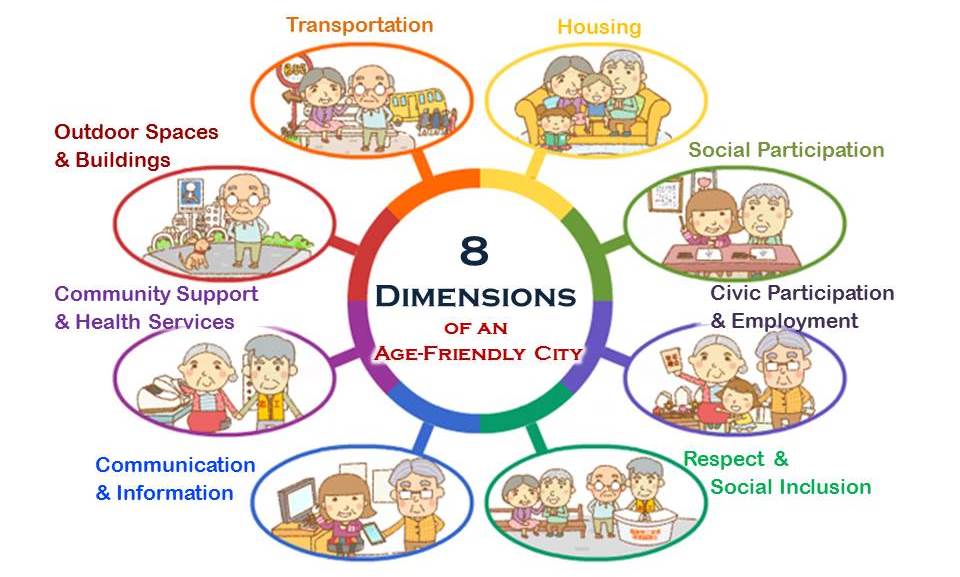
Source of the "8 Dimensions of an Age-Friendly City" diagram: HPA website
Since 2010, the Health Promotion Administration (“HPA”) under the Ministry of Health and Welfare has often referred to the WHO’s 2007 publication of “Global Age-friendly Cities: A Guide” to transform Taiwan into an age-friendly society. The guide has assisted in the review of current living environments for aged citizens and resulted in ideas and suggestions toward a program that expands into eight areas:
- Outdoor spaces and building,
- Transportation
- Housing
- Social participation
- Respect and social inclusion
- Civic participation and employment
- Communication and information
- Community support and health services
Thus far, a total of 22 cities have been implemented and certified as “age-friendly cities” throughout Taiwan, which puts Taiwan as the country with the highest coverage of age-friendly cities.
 The Third Wave of Palliative Care and Hospice Movement
The Third Wave of Palliative Care and Hospice Movement
 Despite the high placement, HPA is not yet content with the current status and is taking the lead to initiate Compassionate Cities Movement. Using WHO’s concept of “Healthy Cities,” palliative care is to be included in a city’s promotion of health. Besides advocating the slogan “staying healthy is everyone’s responsibility,” HPA is also emphasizing the access of quality palliative care and end-of-life care to all elderly to complete the healthy life cycle. What Compassion Cities is stressing is the universal concept that “palliative care and end of life are the basic rights for everyone.”
Despite the high placement, HPA is not yet content with the current status and is taking the lead to initiate Compassionate Cities Movement. Using WHO’s concept of “Healthy Cities,” palliative care is to be included in a city’s promotion of health. Besides advocating the slogan “staying healthy is everyone’s responsibility,” HPA is also emphasizing the access of quality palliative care and end-of-life care to all elderly to complete the healthy life cycle. What Compassion Cities is stressing is the universal concept that “palliative care and end of life are the basic rights for everyone.”
According to a survey, the average YLD (years lived with disability) for Taiwanese citizens is 9-10 years (average age minus healthy years), which is a similar result to most developed countries. However, the average years of healthy life of the Taiwanese is 71 years, which is less than Japan’s 75 years and Korea’s 73 years. How can these healthy years be lengthened and disabled years be reduced? This obviously requires attention to improve the situation.
Be Sick Less, Age Slower, and Live Well
According to WHO’s World Report on Ageing and Health published in 2015, it points out the ideal life course is to still possess appropriate functional abilities before one’s life ends. In other words, what an ideal life requires is to be sick less, age slower, and live well. To achieve this goal, the government should set up a policy to assist the elderly in chronic diseases prevention, early awareness and control, helping the elderly to effectively control or eliminate symptoms while gradually losing functional ability and living with quality.
 When severe dysfunction has already occurred, the goal of care should divert to how chronic diseases can be managed and supported to ensure the dignity of life, and at the same time, link the family caregiver system with the social support system in order to avoid the tragedy of a caregiver’s emotional breakdown.
When severe dysfunction has already occurred, the goal of care should divert to how chronic diseases can be managed and supported to ensure the dignity of life, and at the same time, link the family caregiver system with the social support system in order to avoid the tragedy of a caregiver’s emotional breakdown.
In general, the elderly receive intensive medical services, which can prolong the bedridden period or produce futile results. The Religions of the World Charter – Palliative Care for Older People, published by the Vatican in March 2017, explicitly reports that the elderly ought to have the right of receiving quality palliative care. The life quality of patients should be improved, and respect should be given to an individual’s religion, cultural norms, personal wishes and likings. From a human rights’ perspective, palliative care ought to be
covered by basic medical insurance, and the discrimination against the elderly should be abolished. The elderly are entitled and free to consent, refuse or withhold any medical treatment as they see fit.
 It has become a great challenge for medical professionals to provide complete and comprehensive end-of-life care for the frail elderly. Unlike cancer patients, the frail elderly each has his/her own unique medical history with multiple diseases and mental disabilities. Thus, a personalized care plan for patients and their families is needed and would rely on medical professionals’ detailed prognosis.
It has become a great challenge for medical professionals to provide complete and comprehensive end-of-life care for the frail elderly. Unlike cancer patients, the frail elderly each has his/her own unique medical history with multiple diseases and mental disabilities. Thus, a personalized care plan for patients and their families is needed and would rely on medical professionals’ detailed prognosis.
Reflection on the Co-existence of Illness and Comfort
The goal of palliative care is to improve the quality of life, support the elderly’s functional abilities, and help them face death with dignity. Palliative care not only reflects on the care for illness and comfort, but also supports patients and family members’ social, psychological, and spiritual perspectives. Taiwan’s current palliative care service now includes cancer patients as well as non-cancer patients who have advanced dementia; and service is provided in hospitals, homes, long-term care facilities and communities. The elderly are also encouraged to participate via Advance Care Planning and Shared Decision Making to demonstrate their autonomy and express their free will.
HPA will actively construct a supportive and friendly environment to the elderly and advanced cancer patients, as it seeks to combine age-friendly community, dementia-friendly community, and caring-spirit community. With the joint efforts made by public and private sectors, everyone can expect to live a quality life until the very end.



